Topics
11/21/2019
The Women's Health Initiative Dietary Modification Trial
(References: “The Obesity Code”: Dr. Jason Fung, 2016)
(In the U.S.)The National Institutes of Health recruited almost 50,000 post-menopausal women for the most massive, expensive, ambitious and awesome dietary study ever done. Published in 2006, this randomized controlled trial was called the Women's Health Initiative Dietary Modification Trial. This trial is arguably the most important dietary study ever done.
Approximately one-third of these women received a series of eighteen education sessions, group activities, targeted message campaigns and personalized feedback over one year. Their dietary intervention was to reduce dietary fat, which was cut down to 20 percent of daily calories. They also increased their vegetable and fruit intake to five servings per day and grains to six servings.
They were encouraged to increase exercise. The control group was instructed to eat as they normally did. Those in this group were provided with a copy of the Dietary Guidelines for Americans, but otherwise received little help. The trial aimed to confirm the cardiovascular health and weight-reduction benefits of the low-fat diet.
The average weight of participants at the beginning of the study was 169 pounds (76.8 kilograms). The starting average body mass index was 29.1, putting participants in the overweight category (body mass index of 25 to 29.9), but bordering on obese (body mass index greater than 30). They were followed for 7.5 years to see if the doctor-recommended diet reduced obesity, heart disease and cancer as much as expected.
The group that received dietary counseling succeeded. Daily calories dropped from 1788 to 1446 a dayーa reduction of 342 calories per day for over seven years. Fat as a percentage of calories decreased from 38.8 percent to 29.8 percent, and carbohydrates increased from 44.5 percent to 52.7 percent. The women increased their daily physical activity by 14 percent. The control group continued to eat the same higher-calorie and higher-fat diet to which they were accustomed.
The results were telling. The“Eat Less, Move More”group started out terrifically, averaging more than 4 pounds (1.8 kilograms) of weight loss over the first year. By the second year, the weight started to be regained, and by the end of the study, there was no significant difference between the two groups.
Did these women perhaps replace some of their fat with muscle? Unfortunately, the average waist circumference increased approximately 0.39 inches (0.6 centimeters), and the average waist-to-hip ratio increased from 0.82 to 0.83 inches (2.1 centimeters), which indicates these women were actually fatter than before. Weight loss over 7.5 years of the Eat Less, Move More strategy was not even one single kilogram (2.2 pounds).
This study was only the latest in an unbroken string of failed experiments. Caloric reduction as the primary means of weight loss has disappointed repeatedly.(*snip*)
Many people tell me, “I don't understand. I eat less. I exercise more. But I can't seem to lose any weight.” I understand perfectly-because this advice has been proven to fail.
Do caloric-reduction diets work? No.
(Overeating Experiments: Unexpected Results)
THE HYPOTHESIS THAT eating too much causes obesity is easily testable. You simply take a group of volunteers, deliberately overfeed them and watch what happens. If the hypothesis is true, the result should be obesity.
Luckily for us, such experiments have already been done. Dr. Ethan Sims performed the most famous of these studies in the late 1960s.(*snip*)
Could he make humans deliberately gain weight? This question, so deceptively simple, had never before been experimentally answered. After all, we already thought we knew the answer. Of course overfeeding would lead to obesity.
But does it really? Sims recruited lean college students at the nearby University of Vermont and encouraged them to eat whatever they wanted to gain weight. But despite what both he and the students had expected, the students could not become obese.(*snip*)
Dr. Sims changed course. Perhaps the difficulty here was that the students were increasing their exercise and therefore burning off the weight, which might explain their failure to gain weight. So the next step was to overfeed, but limit physical activity so that it remained constant. For this experiment, he recruited convicts at the Vermont State Prison. Attendants were present at every meal to verify that the caloriesー4000 per dayーwere eaten. Physical activity was strictly controlled
A funny thing happened. The prisoners' weight initially rose, but then stabilized. Though at first they'd been happy to increase their caloric intake, as their weight started to increase, they found it more and more difficult to overeat, and some dropped out of the study.(*snip)
After the experiment ended, body weight quickly and effortlessly returned to normal. Most of the participants did not retain any of the weight they gained.
11/21/2019
Weight Loss Without Rebounding Requires Two Steps
Summary
(1)Just as weight gain does, weight loss likely involves two distinct physiological processes. Under conventional calorie restriction, the body tends to perceive an energy deficit and triggers adaptive responses aimed at maintaining the previous body weight level. As a result, weight loss is difficult to sustain, and body weight often returns to its original range.
To achieve long-term weight loss without rebounding, it is necessary to lower the body’s weight “set-point” itself.
(2)Lowering this set-point likely requires at least two physiological steps.
First, before reducing body weight, it is essential to establish a physiological environment in which the body does not perceive energy deprivation. Second, within that environment, undergo a process where body fat naturally decreases over time.
Step One:
The diet is structured around foods that are nutrient-dense and slow-digesting, such as vegetables, dairy products, nuts, and certain protein-rich foods.
When intestinal contents containing less digestible matter remain in the gut for extended periods, this may be perceived by the body as a signal that food is sufficiently available. As a result, even if overall energy balance becomes slightly negative, strong adaptive responses are less likely to be triggered.
Step Two :
Sustained satiety not only helps prevent overeating, but may also gradually reduce absorption efficiency. Over the long term, coordinated interactions between the brain—particularly the hypothalamus—and peripheral organs and tissues may allow body fat to decline in a stepwise manner.
(3)Although the two-step approach may result in a dietary pattern that resembles a low-carb diet, the underlying goal is fundamentally different.
Low-carb diets primarily aim to reduce insulin secretion by restricting carbohydrate intake. In contrast, the two-step approach focuses on creating a physiological environment opposite to intestinal starvation. To achieve this, it reduces carbohydrate intake while increasing the intake of nutrient-dense foods that take longer to digest, in sufficient amounts.
【Full text】
-
Contents
-
- Two distinct physiological processes underlying weight loss
- What is required to lower the set-point for body weight?
Step one
Step two - How the two-step approach differs from low-carb diets
Although this blog is not intended as a diet guide, examining the mechanisms of weight gain inevitably requires me to also organize, in theoretical terms, the opposite process—how people lose weight.
In this article, I will outline a theory of sustainable weight loss based on my own hypothesis. This discussion is theoretical rather than practice-based, and its purpose is to share a new way of thinking free from conventional constraints.
1. Two distinct physiological processes underlying weight loss
I propose that just as weight gain involves two physiologically distinct processes, weight loss can also occur through two physiologically distinct processes.
(1) Weight decreases, but rebounds
Conventional calorie restriction and low-fat diets are designed to reduce body weight by decreasing energy intake and increasing energy expenditure. This approach often involves constant hunger.
In this blog, I use the body weight set-point hypothesis[1,2] as a framework to explain weight homeostasis.
When energy intake is severely restricted and body weight decreases, the body perceives an energy deficit and triggers adaptive responses aimed at preserving stored energy[3,4].
These responses are best understood as adaptive processes that consist of interacting changes in metabolism, neuroendocrine function, autonomic regulation, and behavior[5].
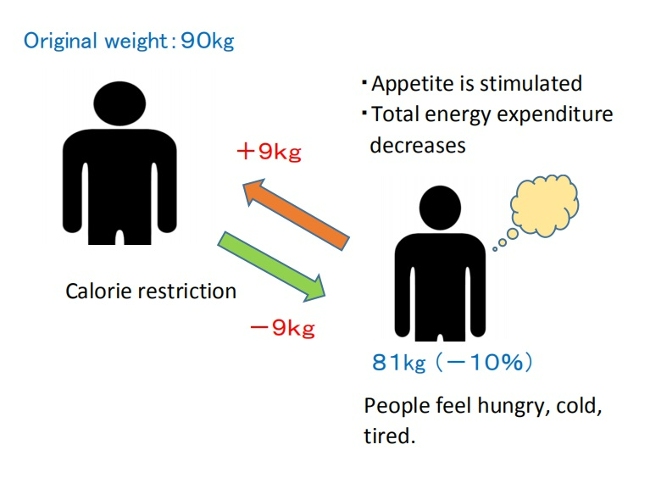
In addition, in my opinion, prolonged hunger leads the body to extract as much nutrition as possible from food, thereby increasing absorption efficiency.
In most cases, however, the body’s weight set-point itself does not change. As a result, weight loss is not sustained, and body weight is likely to return to its original range over time.
【Related article】
Biological Responses Driving Weight Rebound After Weight Loss
(2) Lowering the body weight “set-point” itself
I believe that the fundamental problem in obesity lies in an elevated body weight set-point.
Even though obese individuals have ample energy stores, they still exhibit metabolic resistance to caloric restriction, suggesting that obesity represents a physiologically stable state for some people[1]. Animal studies similarly describe obesity as a condition of energy homeostasis regulated around a higher set-point[1].
Therefore, achieving long-term weight loss requires not merely focusing on short-term energy balance, but lowering the body weight set-point itself. Relevant literature supporting this perspective is cited below.
"There appears to be a “set point” for body weight and fatness, and the problem in obesity is that the set point is too high.(*snip*)
There are two prominent findings from all the dietary studies done over the years.
First: all diets work. Second: all diets fail.
What do I mean?
Weight loss follows the same basic curve so familiar to dieters. Whether it is the Mediterranean, the Atkins or even the old fashioned low-fat, low-calorie, all diets in the short term seem to produce weight loss. Sure, they differ by amount lost–some a little more, some a little less. But they all seem to work.
However, by six to twelve months, weight loss plateaus, followed by a relentless regain, despite continued dietary compliance.(*snip*)
So all diets fail. The question is why.
Permanent weight loss is actually a two-step process. There is a short-term and a long-term (or time-dependent) problem. "
( Fung J. 2016. The obesity code. pages 62,215 )
2. What is required to lower the set-point for body weight?
In my understanding, the “two-step process” described by Doctor Fung is a conceptual framework that views obesity treatment (weight loss) as consisting of a short-term and a long-term challenge, organized primarily from a clinical and practical perspective.
On the other hand, this article focuses on the long-term problem—specifically, why the body resists weight loss and why body weight,once reduced, often returns over time[6]—and explores this issue more deeply from a physiological perspective.
Based on this analysis, I suggest that successful long-term weight loss requires at least the following two physiological steps:
(1) Before trying to lose weight, creating a physiological state in which the body does not perceive energy deprivation.
(2) Within that state, allowing body fat to decrease naturally over time.
My theory posits that weight gain accompanied by an upward shift in the body’s set-point weight is closely related to adaptive responses that arise when the body perceives a state of starvation. Therefore, I believe that reducing body weight in a sustained manner require creating the opposite physiological environment.
Many diets aim for losing weight from the very beginning. However, when the first step is skipped, the body tends to activate adaptive responses to restore homeostasis[6], which can increase the likelihood of long-term weight rebound.
Specifically, the process can be described as follows.
Step one
Rather than reducing overall food intake and enduring hunger, this approach centers the diet around nutrient-dense foods that either take longer to digest or are partially indigestible.
More specifically, this involves reducing the intake of refined carbohydrates and instead increasing consumption of foods such as whole grains, fiber-rich vegetables, nuts, dairy products, fat, and minimally processed protein foods.

Author: brgfx. Source: Freepik
As a result, intestinal contents that include less easily digestible matter remain in the gut for a longer period of time. This may not only reduce the sensation of hunger but also may be perceived by the body as a signal that food is sufficiently available. Consequently, even if overall energy balance becomes slightly negative, the body is less likely to perceive this state as energy deprivation.
Step two
As hunger diminishes, appetite tends to decrease, and absorption efficiency may also gradually decline. Eventually, I suggest that coordinated interactions between the brain—centered on the hypothalamus—and peripheral organs and tissues[7] may contribute to a gradual reduction in body fat.
Changes in absorption efficiency may not be intuitive at first glance, but consider this: consuming carbohydrates in a state of intense hunger tends to cause a rapid rise in blood glucose levels, whereas eating them several hours after a meal moderates the rise. Similarly, alcohol intoxication occurs faster on an empty stomach, but more gradually after eating.
Thus, by avoiding prolonged hunger and consuming foods that require longer digestion at appropriate intervals, absorption efficiency may gradually decrease in relative terms.
3. How the two-step approach differs from low-carb diets
The “two-step approach” proposed here may, in practice, result in a dietary pattern that resembles a low-carbohydrate diet. However, the two differ fundamentally in their starting points and underlying goals. In this section, I will clarify these differences.
▽Low-carb diets primarily aim to limit carbohydrate intake in order to suppress rapid spikes in blood glucose and reduce insulin secretion, which plays a key role in fat storage.
When energy derived from carbohydrates becomes insufficient, the body shifts to using fat as its main energy source, entering what is known as a state of ketosis. As a result, body fat tends to be utilized more readily, and body weight may decrease relatively quickly.
Another commonly cited feature of low-carb diets is that they do not require strict calorie counting, and often promote satiety through higher protein and fat intake.
▽In contrast, my own theory likewise considers diets heavily skewed toward refined carbohydrates and highly processed foods to be likely contributors to the modern obesity epidemic. However, this is not because carbohydrates themselves are inherently harmful in a direct sense.
What I emphasize instead are certain properties of carbohydrates: their rapid digestibility; the “dilution effect” that occurs when carbohydrates are consumed together with large amounts of water; and the “push-out effect,” whereby gastric contents are rapidly propelled into the intestine.

Author: brgfx. Source: Freepik
When these factors act together, all ingested food may be digested and expelled relatively quickly, potentially increasing the likelihood of intestinal starvation under specific conditions.
【Related article】
The Dilution Effect/ Pushing Out Effect of Carbohydrates
For this reason, the two-step approach aims to create a physiological environment opposite to intestinal starvation—namely, a state in which intestinal contents containing less digestible matter remain in the gut for an extended period. To achieve this, carbohydrate intake is reduced in order to weaken the dilution and push-out effects, while the relative intake of other foods—such as fiber-rich vegetables, dairy products, fats, and minimally processed protein sources—is increased.
In low-carb diets, by contrast, the central strategy is to reduce carbohydrate intake itself, while proteins and fats are consumed relatively freely as alternative energy sources. This distinction represents a fundamental difference between low-carb diets and the two-step approach described here.
References
[1]Richard E. Keesey, Matt D. Hirvonen, Body Weight Set-Points: Determination and Adjustment, The Journal of Nutrition, Volume 127, Issue 9, 1997, Pages 1875S-1883S, ISSN 0022-3166.
[2]Ganipisetti VM, Bollimunta P. Obesity and Set-Point Theory. 2023 Apr 25. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan–.
[3]Hall KD, Guo J. Obesity Energetics: Body Weight Regulation and the Effects of Diet Composition. Gastroenterology. 2017 May;152(7):1718-1727.e3.
[4]Egan AM, Collins AL. Dynamic changes in energy expenditure in response to underfeeding: a review. Proc Nutr Soc. 2022 May;81(2):199-212.
[5] Rosenbaum M, Leibel RL. Adaptive thermogenesis in humans. Int J Obes (Lond). 2010 Oct;34 Suppl 1(0 1):S47-55.
[6] Ochner CN et al. Biological mechanisms that promote weight regain following weight loss in obese humans. Physiol Behav. 2013 Aug 15;120:106-13.
[7] Wilson JL, Enriori PJ. A talk between fat tissue, gut, pancreas and brain to control body weight. Mol Cell Endocrinol. 2015 Dec 15;418 Pt 2:108-19.
08/14/2019
How Intestinal Starvation Can Lead to Weight Gain
-
Contents
-
- Hunger in Africa and a modern form of hunger
- Adaptive responses to intestinal starvation
- What happens when the body shifts to a higher body-weight set point?
(1) Once weight is gained, it becomes harder to lose
(2) Muscle mass also increases concurrently
(3) A reversal of cause and effect
Introduction
In this article, I will discuss the central theme of this blog: why a state I call “intestinal starvation” can lead to weight gain. This idea is based on my own personal experience, which I have organized and interpreted from a physiological perspective and presented here as a hypothesis.
When I entered university, my body weight had dropped into the 30-kilogram range. Even when I increased my food intake, my weight barely increased.
However, at one point, despite eating relatively little, my body weight suddenly increased by about five kilograms over the course of four to five days. This increase involved not only body fat but also muscle mass. Because I was underweight at the time, I strongly felt that this rapid weight gain was not a coincidence but rather the result of a distinct physiological change.
The idea presented in this article may seem counterintuitive to many readers. Nevertheless, for those who feel that weight gain cannot be fully explained by calorie balance alone, I hope this perspective offers a useful way of thinking.
1. Hunger in Africa and a modern form of hunger
The idea that humans have evolved to store fat more efficiently in preparation for temporary food shortages or famine is one that most researchers studying obesity have likely considered at least once. However, this simple hypothesis has historically been treated with caution—or even skepticism—within the scientific community[1].
Underlying this skepticism is the common observation that people with obesity tend to have a higher energy intake, whereas individuals experiencing severe famine, such as refugees in parts of Africa, are markedly underweight due to malnutrition. From this perspective , some may raise the following counterargument:
“If hunger leads to weight gain, then refugees in Africa should be overweight.”

Image credit: macrovector / Freepik
However, this represents starvation—conditions in which people want to eat but cannot.
Under such extreme circumstances, the body does not first store fat; instead, muscle mass is lost and basic physiological functions begin to decline. Digestive and absorptive capacity itself may be impaired, leaving the body with little ability to store energy at all.
▽In contrast, the term “intestinal starvation,” as used here, refers to a physiological state in which the body perceives the absence of food when the contents of the gastrointestinal tract have been almost completely digested.
This condition can be regarded as a modern form of hunger that began to emerge primarily in developed countries around the 1970s and has since been spreading to many parts of the world.
In developed countries, diets have increasingly shifted toward the routine consumption of high-calorie, highly processed foods. In particular, when a diet is consistently dominated by rapidly digestible refined carbohydrates and (ultra-)processed foods, undigested matter does not remain in the intestinal tract for extended periods, which may create conditions that make intestinal starvation more likely to occur.
In fact, obesity has become a serious problem even among some low-income populations worldwide[2]. What is commonly observed in these settings is not simply excessive caloric intake or high sugar consumption, but rather a poorly balanced diet heavily reliant on inexpensive refined carbohydrates and highly processed foods.
2. Adaptive responses to intestinal starvation
I propose that one of the fundamental problems underlying obesity is that the body-weight set point is elevated. I further suggest that this upward shift in the set point may involve adaptive responses that are triggered when the body, in some form, perceives a state of starvation.
In this section, I will explain the concept of intestinal starvation—one form of perceived starvation—and the process by which it may lead to weight gain, using an analogy from plant biology. (Note that the discussion here is limited to intestinal starvation and does not attempt to explain other known or unknown mechanisms involved in weight gain.)

Image credit: brgfx / Freepik
When plants are placed in nutrient-poor environments, they extend their roots deeper into the soil in order to obtain more nutrients.
Similarly, I propose that in humans, when all ingested food is almost completely digested throughout the intestines—primarily the small intestine—and the body perceives a state in which “no food is present,” that is, when intestinal starvation occurs, a similar adaptive response may be triggered.
Having said that, it should be emphasized that this does not imply that the protrusions on the intestinal folds—the villi—physically elongate. What I am proposing is not a change in the intestinal structure or function itself, but rather more superficial changes that influence absorptive efficiency.
The interior of the small intestine has an extremely large absorptive surface area due to its folded structure, countless villi, and the microvilli that develop on the surface of each villus (Figure 1).
When fully spread out, the surface area of the small intestine is often said to be equivalent to that of a tennis court.
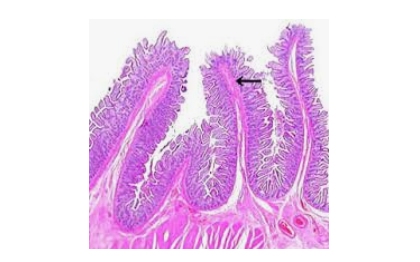
Fig. 1. Intestinal villi
My hypothesis is that when a signal indicating the absence of food is transmitted from the intestines—particularly the small intestine—to the central nervous system, the body is adjusted toward securing more nutrients.
In this process, as an adaptive response, microscopic particles (e.g. matter derived from food residue) adhering to the surface of the villi and microvilli may be sloughed off and are released into the intestinal contents (Figure 2).
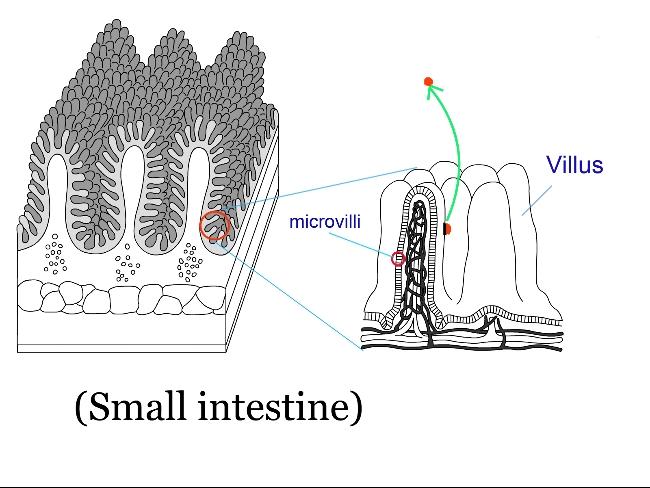
Fig. 2. Adaptive responses to intestinal starvation
As a result, the surface area available for contact with nutrients increases, and the effective absorptive efficiency may rise in a way that is not merely transient but can persist thereafter.
If such a change in absorptive efficiency occurs, regardless of whether the weight gain is 0.3 kg or 3 kg, the body may transition to a state of energy homeostasis at a higher body weight within a relatively short period of time. Unlike weight gain caused by overeating, this would imply an upward shift in the body-weight set point itself.
This hypothesis may help explain, at least in part, why individuals with obesity—despite having substantial energy stores in the form of body fat—can exhibit metabolic resistance to caloric restriction[3].
【Related articles】The Increasingly Important "Set-Point" Theory of Body Weight
Taken together, I propose that one fundamental difference between obese and lean individuals may lie in how efficiently ingested food is digested and absorbed.
In Japan, people with obesity sometimes describe themselves as “having a body that gains weight even from drinking water.” Of course, drinking water alone does not lead to weight gain. However, this expression may intuitively reflect a state in which nutrient absorption efficiency is elevated in individuals with obesity.
3. What happens when the body shifts to a higher body-weight set point?
(1) Once weight is gained, it becomes harder to lose
Weight gain reflecting an elevation of the body-weight set point means, from the perspective of energy homeostasis, that the balance point at which energy intake and expenditure are matched has shifted to a higher level. In other words, a more positive energy balance becomes easier to maintain, making weight loss increasingly difficult.
Even if body weight temporarily decreases through caloric restriction, it is highly likely to rebound once the original diet is resumed.
Moreover, repeated cycles of dietary restriction may raise concerns about a gradual increase in body weight over the long term. With extreme dietary restriction, prolonged periods of hunger are common, which may make intestinal starvation more likely to occur during this process and, in turn, further elevate the set point for body weight.
(2) Muscle mass also increases concurrently
In weight gain reflecting an upward shift in the body-weight set point, the efficiency of absorption of nutrients as a whole, including protein, may increase.
Consequently, not only body fat but also fat-free tissues—such as muscle and organs—may increase in parallel to a certain extent.
Indeed, many studies have reported that individuals with obesity tend to have greater fat-free mass (including muscle mass) than non-obese individuals[4,5,6,7].

Image credit: Pikisuperstar/ Freepik
However, these findings are primarily observational and do not demonstrate that the increase in body fat itself—or the associated increase in body weight load—directly stimulates muscle growth.
In this hypothesis, increases in muscle mass are not attributed to mechanical loading from higher body weight. Rather, they are considered to occur alongside increases in body fat to some extent as a secondary change associated with alterations in nutritional status and the metabolic environment.
(3) A reversal of cause and effect
An increase in overall nutrient uptake shifts the body toward a more positive energy balance, while simultaneously allowing the following phenomena to occur. Since digestive enzymes and many hormones are composed of proteins (amino acids), improvements in nutritional status may lead to changes in digestive function and appetite regulation mechanisms.
As a result, it is natural that individuals with larger body size or higher digestive capacity tend to consume larger amounts of food.
In other words, it is not that “eating more causes weight gain,” but rather that as the body becomes larger, its energy needs increase, which in turn leads to a tendency to eat more.
From this perspective, the relationship between cause and effect can be understood as being reversed.

Source: Freepik
In contrast, in an excessively lean state, reduced absorptive efficiency may limit the body’s ability to effectively utilize ingested nutrients, such as protein. As a result, decreases in the muscle mass that supports internal organs, together with reduced secretion of digestive enzymes, can further impair the capacity to digest and absorb food efficiently.
This creates a vicious cycle in which a negative energy balance is more easily maintained. Consequently, even when caloric intake is increased, body weight may not increase easily.
【Related articles】
After Gaining Weight, We Eat Too Much and Do Less Exercise
References
[1]Speakman JR, Elmquist JK. Obesity: an evolutionary context. Life Metab. 2022 Apr 29;1(1):10-24.
[2]Gary Taubes. Why We Get Fat. New York: Anchor Books. 2011. Pages 15-32.
[3]Richard E. Keesey, Matt D. Hirvonen, Body Weight Set-Points: Determination and Adjustment, The Journal of Nutrition, Volume 127, Issue 9, 1997, Pages 1875S-1883S, ISSN 0022-3166.
[4]Kyle UG et al. Fat-free and fat mass percentiles in 5225 healthy subjects aged 15 to 98 years. Nutrition. 2001 Jul-Aug;17(7-8):534-41.
[5]Heymsfield SB et al. Human body composition: advances in models and methods. Annu Rev Nutr. 1997;17:527-58.
[6] Janssen I et al. Skeletal muscle mass and distribution in 468 men and women aged 18-88 yr. J Appl Physiol (1985). 2000 Jul;89(1):81-8.
[7]Fornari R et al. Lean mass in obese adult subjects correlates with higher levels of vitamin D, insulin sensitivity and lower inflammation. J Endocrinol Invest. 2015 Mar;38(3):367-72.
06/22/2019
Obesity as a Multifactorial Condition: Does Intestinal Starvation Act as a Confounding Factor?
-
Contents
- "Overeating causes obesity" is too simplistic
- Most diet methods are "partially correct"
- Can environmental and behavioral factors be systematically organized?
- Intestinal starvation as a confounding factor
The bottom line
1. "Overeating causes obesity" is too simplistic
A 2012 online survey of 1,143 adults in the United States conducted by Reuters and the market research firm Ipsos found that 61% of American adults believed "personal choices related to diet and exercise" were responsible for the obesity epidemic[1,2]. In other words, many Americans still hold the belief that people who become obese lack willpower, overeat, and do not exercise enough[2].
The situation in Japan appears to be similar. Even news anchors and experts frequently make statements such as, “It's only natural to gain weight if you overeat and don’t exercise,” suggesting that many Japanese people likely hold the same view.
However, scientific research indicates that "personal choices" may not account for all cases of obesity[2].
Classical genetic studies based on adoption studies, family studies, twin studies, etc., indicate that about 50–70% of the variance (heritability estimates) in BMI is genetic (Those estimates vary depending on the study design and assessment methods) [3].
Even today, the heritability of obesity is estimated at 40% to 70%[4].

Some researchers point out that numerous different genes have been found to be involved in food selection, food intake, absorption, metabolism, and energy expenditure including physical activity. When considering interactions between gene-by-gene or gene(s)-by-environment(s), the complexity of the mechanisms underlying weight regulation becomes even greater[3].
International Statements Recognizing Obesity as a Chronic Disease
・In 1948, the World Health Organization (WHO) established the International Classification of Diseases (ICD) and classified obesity as a disease. This is considered one of the earliest official frameworks in which obesity was treated as an illness.
However, at the time, this classification received little attention within the medical community and was not widely regarded as clinically important for several decades thereafter[5].
・In 1997, following consultations with the International Obesity Task Force (IOTF, now part of the World Obesity Federation), the WHO clearly identified obesity as a complex and serious chronic disease in an official report[6].
・In 2012, the American Association of Clinical Endocrinologists (AACE) designated obesity as a chronic disease. This designation was based on the recognition that the pathophysiology of obesity is complex, involving interactions among genetic and biological factors, the environment, and behavior, and that obesity meets the definition of a disease as outlined by the American Medical Association (AMA)[7].
・Subsequently, in 2013, the American Medical Association (AMA) formally recognized obesity as a chronic disease[8].
2. Most diet methods are partially correct
If we accept that the human gene pool is unlikely to change substantially over a period of 50 or even 100 years, then the global rise in obesity observed since the 1970’s can reasonably be understood as being strongly influenced by environmental and behavioral factors.
With this in mind, I would like to take a closer look at these factors. An interesting observation about recent popular diets is particularly relevant here and is quoted below.
“What causes weight gain? Contending theories abound:
・Calories ・Food reward・Food addiction
・Sugar・Sleep deprivation ・Stress
・Refined carbohydrates・Wheat
・Low fiber intake・All carbohydrates
・Genetics・Dietary fat ・Red meat
・Poverty ・All meat・Wealth
・Dairy products・Gut microbiome
・Snacking・Childhood obesity

The various theories fight among themselves, as if they are all mutually exclusive and there is only one true cause of obesity. For example, recent trials that compare a low-calorie to a low-carbohydrate diet assume that if one is correct, the other is not. Most obesity research is conducted in this manner.
This approach is wrong, since these theories all contain some element of truth. (*snip*)
THE MULTIFACTORIAL NATURE of obesity is the crucial missing link. There is no one single cause of obesity. (*snip*)
What we need is a frame work, a structure, a coherent theory to understand how all its factors fit together. Too often, our current model of obesity assumes that there is only one single true cause, and that all others are pretenders to the throne. Endless debates ensue.
Too many calories cause obesity. No, too many carbohydrates. No,
too much saturated fat. No, too much red meat. No,
too much processed foods. No, too much high fat dairy. No,
too much wheat. No, too much sugar. No,
too much highly palatable foods. No, too much eating out. No
It goes on and on. They are all partially correct. (*snip*)
All diets (e.g., calorie restriction, low-fat, paleo, vegan) work because they all address a different aspect of the disease. But none of them work for very long, because none of them address the totality of the disease.
Without understanding the multifactorial nature of obesity-which is critical -we are doomed to an endless cycle of blame."
(Jason Fung. The Obesity Code. Greystone Books. 2016. Pages 70, 216-217.)
I find the author’s discussion of the multifactorial nature of obesity to be highly insightful. Obesity is not a simple phenomenon caused solely by overeating; rather, it arises from a complex interplay of multiple factors, and this is a point we must first recognize.
However, at the same time, the sheer number of factors that are often listed suggests another problem: the mechanisms and contributing factors behind weight gain have not been sufficiently organized or clearly conceptualized.
I believe that by introducing the concept of intestinal starvation, some of the environmental and behavioral factors that appear complex can be viewed in a more structured and coherent way. By shifting our focus away from observable eating habits and lifestyle patterns and toward the unseen workings of the intestines, the underlying mechanisms of obesity may become more apparent.
3. Can environmental and behavioral factors be systematically organized?
Here, it is worth reaffirming that the phenomenon commonly described as “gaining weight” actually involves two distinct processes. Introducing this conceptual framework makes it easier to organize and understand the many factors that contribute to weight gain.
【Related article】
The Two Distinct Processes Behind Weight Gain
(1) When body weight returns to its original set point
One type of weight gain occurs when body weight, which has been intentionally kept low, begins to return toward its set point. This process is illustrated in Figure 1A.
Not only the weight gain commonly explained as resulting from overeating or lack of exercise, but also many calorie-restricted diets and traditional weight-loss intervention studies fall into this category.
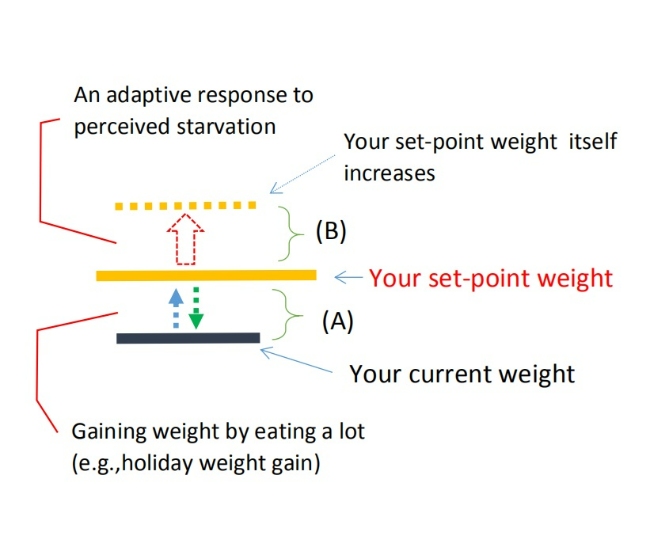
Fig. 1
Admittedly, regardless of whether fat, carbohydrates, or ultra-processed foods are restricted, body weight tends to decrease temporarily as long as energy intake falls below energy expenditure.
However, because this approach does not alter the underlying body-weight set point, making long-term weight loss maintenance difficult and increasing the likelihood of weight rebound once previous eating patterns resume.
As Dr. Briffa has pointed out, calorie restriction may serve as a temporary remedy, but it is not a fundamental solution to obesity as a whole.
(2) The process by which the set point itself increases
In contrast, the weight gain illustrated in Figure 1B represents a situation in which the body-weight set point itself increases. I propose that this type of weight gain is the result of an adaptive response to the body’s recognition of “starvation.”
One form of this “perceived starvation” is intestinal starvation. Intestinal starvation does not arise from a single cause; rather, it emerges through the simultaneous involvement of multiple factors. This perspective may help clarify the multifactorial nature of obesity, particularly its relationship with environmental and behavioral factors.
【Related article】
Three (+1) Factors That Accelerate “Intestinal Starvation”
4. Intestinal starvation as a confounding factor
Skipping breakfast, eating late dinners, having fewer meals per day, diets high in refined carbohydrates or (ultra-)processed foods, insufficient dietary fiber, and unbalanced diets are often reported to be associated with weight gain and obesity.
What is important, however, is that these factors may not independently cause obesity. Instead, they may influence the occurrence of intestinal starvation.
In other words, I suggest that the core causal factor in obesity may not be individual lifestyle behaviors themselves, but rather intestinal starvation, which is commonly affected by these behaviors.
In this sense, intestinal starvation may be conceptualized as a physiological response that functions as a confounding factor (see Note 1) in obesity research.
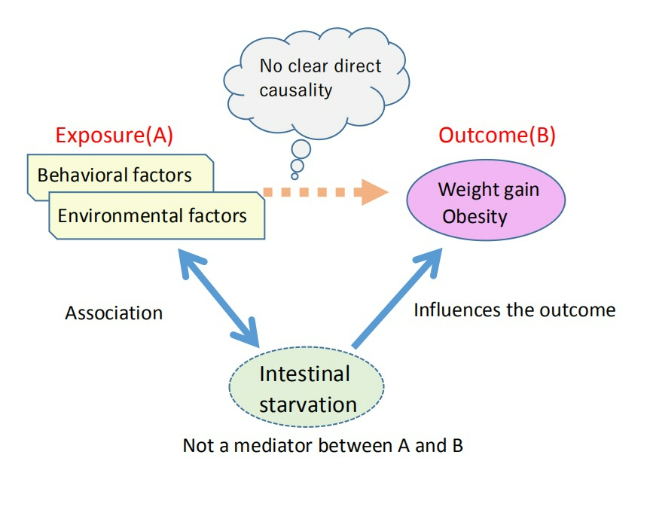
Fig. 2. Conceptual framework of intestinal starvation acting in a confounding-like manner
Note 1: A confounding factor is a third variable that influences both the presumed cause (exposure) and the outcome, thereby obscuring the true relationship between them. For example, even if low dietary fiber intake appears to be associated with obesity, intestinal starvation may be an underlying factor that affects both.
The bottom line
(1)Obesity is now widely recognized as a chronic, multifactorial disease driven by interactions among genetic, biological, environmental, and behavioral factors. While many fad diets address specific aspects of obesity, none adequately targets the condition as a whole, which may explain their limited long-term effectiveness.
(2)What is needed now is a conceptual framework that explains how multiple factors interact. By adopting the perspectives outlined below, environmental and behavioral factors related to obesity can be more clearly organized and understood.
(a) There are two distinct processes that lead to weight gain, and one of them—an upward shift in the body-weight set point—is closely associated with the rise in obesity.
(b) Intestinal starvation is involved in this upward shift of the set point itself. It represents an adaptive physiological response that arises at the intersection of genetic factors and the modern food environment and lifestyle, and thus may help explain the multifactorial nature of obesity.
(3) From this perspective, the central causal factor in obesity may not be individual lifestyle behaviors themselves, but rather intestinal starvation, which is commonly influenced by these factors. In this sense, intestinal starvation can be viewed as a biological response that functions as a confounding factor in obesity research.
References
[1]Begley S. America's hatred of fat hurts obesity fight. Reuters. May 11, 2012.
[2]Jou C. The biology and genetics of obesity--a century of inquiries. N Engl J Med. 2014 May 15;370(20):1874-7.
[3]Speakman JR et al. Set points, settling points and some alternative models: theoretical options to understand how genes and environments combine to regulate body adiposity. Dis Model Mech. 2011 Nov;4(6):733-45.
[4]McPherson R. Genetic contributors to obesity. Can J Cardiol. 2007 Aug;23 Suppl A(Suppl A):23A-27A.
[5]James, W. WHO recognition of the global obesity epidemic. Int J Obes 32 (Suppl 7), S120–S126 (2008).
[6]Obesity as a Disease.The World Obesity Federation
[7] Garvey WT. Is Obesity or Adiposity-Based Chronic Disease Curable: The Set Point Theory, the Environment, and Second-Generation Medications. Endocr Pract. 2022 Feb;28(2):214-222.
[8] Garvey WT et al. American Association of Clinical Endocrinologists and American College of Endocrinology Comprehensive Clinical Practice Guidelines for Medical Care of Patients with Obesity. Endocr Pract. 2016 Jul;22 Suppl 3:1-203.
01/04/2019
The Dilution Effect/ Pushing Out Effect of Carbohydrates: Does This Cause People To Gain Weight?
Contents
- If there were no carbohydrates
- Meals high in indigestible foods are not fattening
- The effect of carbohydrates that make it easier to gain weight
(1) Dilution effect
(2) Pushing out effet
<The bottom line>
When we consider that “eating a lot leads to gaining weight,” I believe you have the image of carbohydrates like bread, rice, and noodles in mind.

This time, I am going to explain the reason why carbohydrates (*1) make it easier for people to gain weight, not because of an increase in calories or of its tendency to raise blood sugar levels, but by other indirect ways.
(*1) Although technically sugar is also a sort of carbohydrate, I use the word carbohydrate here to mean “polysaccharide” such as starches, bread, and rice.
1. If there were no carbohydrates
When my total body weight fell to under forty kilograms, it would have been impossible to have gained weight without the help of carbohydrates. In my case, neither fat nor sugar could have done that … In other words, I would never have gained weight by eating cream-filled cakes or oily pork cutlets and fatty Chinese food. Next, I am going to explain the reason why.
First, not all carbohydrates are the same. Carbohydrates are mainly categorized by their chemical structure into monosaccharides, disaccharides, oligosaccharides, and polysaccharides.
However, substances like cellulose (a polysaccharide), which is treated as dietary fiber, non-digestible oligosaccharides and resistant starch, should be consumed to improve health.
Additionally, while simple carbohydrates like sugar may lead to temporary weight gain or blood sugar-related disorders, I believe they are not a cause of weight gain in the sense that they increase one’s set-point weight.

In terms of increasing the body's set-point weight, I believe the cause of weight gain is the consumption of easily digestible carbohydrates that are high in starch (polysaccharides) and low in dietary fiber, such as refined grains like rice and wheat, and potatoes.
Therefore, foods like brown rice, wholegrain bread, fried rice, and cold rice, while being the same type of carbohydrate, may produce different results.
These are known as low G.I. foods, which don't raise blood sugar levels easily, or resistant starches. In other words, these foods contain many indigestible components or take longer to digest and absorb.
2. Meals high in indigestible foods are not fattening
When you constantly consume foods that are less digestible or slowly digested and absorbed-such as the above-mentioned carbohydrates that don’t raise the blood sugar level, tough meats, fat, fibrous vegetables, seaweed, and dairy product-intestinal starvation is less likely to occur and you are less likely to gain weight, which means the set-point for body weight is unlikely to go up.

I’m simply saying that it is hard to gain weight if a lean person eats them properly every day.
Although a person who is already overweight may not lose weight by eating some less digestible foods, I consider that it may be possible to lose weight depending on how you eat them, since these foods are always discussed in dieting techniques.
3. The effect of carbohydrates that make it easier for people to gain weight
On the contrary, digestible refined carbohydrates that are high in starch (rice, rice porridge, white bread, potatoes, etc.) and processed starches extracted from plants promote overall digestion. By eating them together with digestible proteins, they make it easier to induce intestinal starvation.
Those are two effects that I can think of so far.
(1) Dilution effect
If you proportionally increase digestible carbohydrates (rice, noodles, bread, etc.) in the meal, the percentage of side dishes such as fat, meat, fish, and vegetables will be relatively smaller. The density of a spoonful of oil will be lower if you eat more bread or rice portions with soup (water).

When you eat some meat together with a slice of bread and soup, the density of the meat will be lower.
In other words, easily digestible carbohydrates and water are added and mixed in the stomach, and then the diluted nutrients are sent to the intestines. So, it will be easier to get hungry and induce intestinal starvation.
For example, let’s say you eat a hamburger and a potato, plus another piece of bread and tea. If we mix all of these in a blender, it will be something like meat diluted with starch and water.

In contrast, if we remove the bread and add mixed beans-mayonnaise salad… the dilution effect of carbohydrates will be less, and fiber and fat will be added.
On a caloric basis, mixed beans-mayonnaise salad is, e.g. 100kcal. However, adding it to the meal doesn’t have the same meaning as adding another piece of bread. This is why calorie intake basis thinking may go wrong.

Moreover, as seen in low-carb diets, what would happen if you decrease the intake of carbohydrates in the meal and instead increase proteins such as meat and fish, fat, and vegetables, etc.?
In this case, the opposite effect of the dilution effect occurs: dense nutrients are delivered to the intestines, which slows digestion and undigested food always remains in the gastrointestinal tract.
(2) Pushing out effect

"Balloon effect"
Starch-rich carbohydrates, when consumed with water, cause stomach bloating (I’ll call this the “balloon effect” of the stomach). And, if we eat carbs together with digestible side dishes such as stew (onion, potatoes, low-fat chicken, etc.), its holding time in the gut will be shorter since it’s easy to digest, and the food will be pushed out of the stomach fairly soon. Also, our intestines start to move actively and smoothly.

I had the problem with my stomach and intestines and often suffered from constipation or diarrhea.
But, when I ate Japanese soba noodles(*2) and small rice bowl dishes (chicken and egg over rice), it promoted regular bowel movements and relieved my symptoms several times.
(*2) If you don't know much about soba, it may be easier to imagine ramen noodles without oil.
On the other hand, you may think that eating fatty foods or deep-fried foods give us stamina. It actually means that those foods fill us up better than carbs do, and its energy could be sustained during sports such as a marathon or a soccer match.
That is to say, undigested foods stay longer in our stomach and intestines, so it’s more difficult to induce intestinal starvation.
The bottom line
(1) Simply put, incorporating fibrous foods and slow-digesting foods in your diet makes you less likely to gain weight compared to other meals with the same caloric content.
On the other hand, combining easily digestible foods (such as refined carbohydrates, proteins, and ultra-processed foods) in your diet makes you more likely to gain weight.
(2) Carbohydrates are generally classified into monosaccharides, disaccharides, oligosaccharides, and polysaccharides, depending on their chemical structure.
Substances like cellulose (polysaccharides) which are considered dietary fiber, non-digestible oligosaccharides, and resistant starch, would not cause weight gain and should be consumed to promote health.
I also believe that simple carbohydrates like sugar may cause an increace in blood sugar levels and temporary weight gain, but they are not a cause of weight gain in the sense that they increase one’s set-point weight.
(3) In terms of increasing the body's set-point weight, I believe the foods that may cause obesity are easily digestible carbohydrates (polysaccharides) high in starch, such as white rice, white bread, noodles, and potatoes.
These foods expand with water in the stomach (balloon effect) and may have a "dilution effect" or "push-out effect" in the digestive process, which might lead to intestinal starvation.
(4) Obesity among poverty-stricken people worldwide can be understood as the influence of cheap refined carbohydrates and unbalanced diets (lack of vegetables, etc.). Considering them, it may be easier to imagine that they are not gaining weight due to taking too many calories or sugar, but rather from consuming cheap carbohydrates as mentioned above.
[Related article] Wealthy People Get Fat? Poor People Get Fat?

